
Blog
The 5 Senses in Neurology: A Patient Guide to Sensory Loss

Our five senses are how we connect and communicate with the world around us. If you have been blessed to experience all five senses, consider the advantages that you’ve been able to experience in your lifetime. The taste of various flavors, the sound of musical notes, the colors of a South Florida sunset, the warm touch of a loved one, and the aroma of a fresh cup of coffee in the morning.
When it comes to the sensory experience, we rarely give a second thought to its functioning or impermanence in our daily lives. Today, it is estimated that nearly 94 percent of individuals in the US over the age of fifty-seven experience some form of sensory impairment. Age-related sensory loss is a contributing factor often correlated to decreased quality of life.
The Five Senses in Neurology
The brain is the most complex organ of our bodies, comprised of millions of neurological pathways, making processing and communication possible. Any disruptions in these neurological connections can result in loss of communication and functioning.
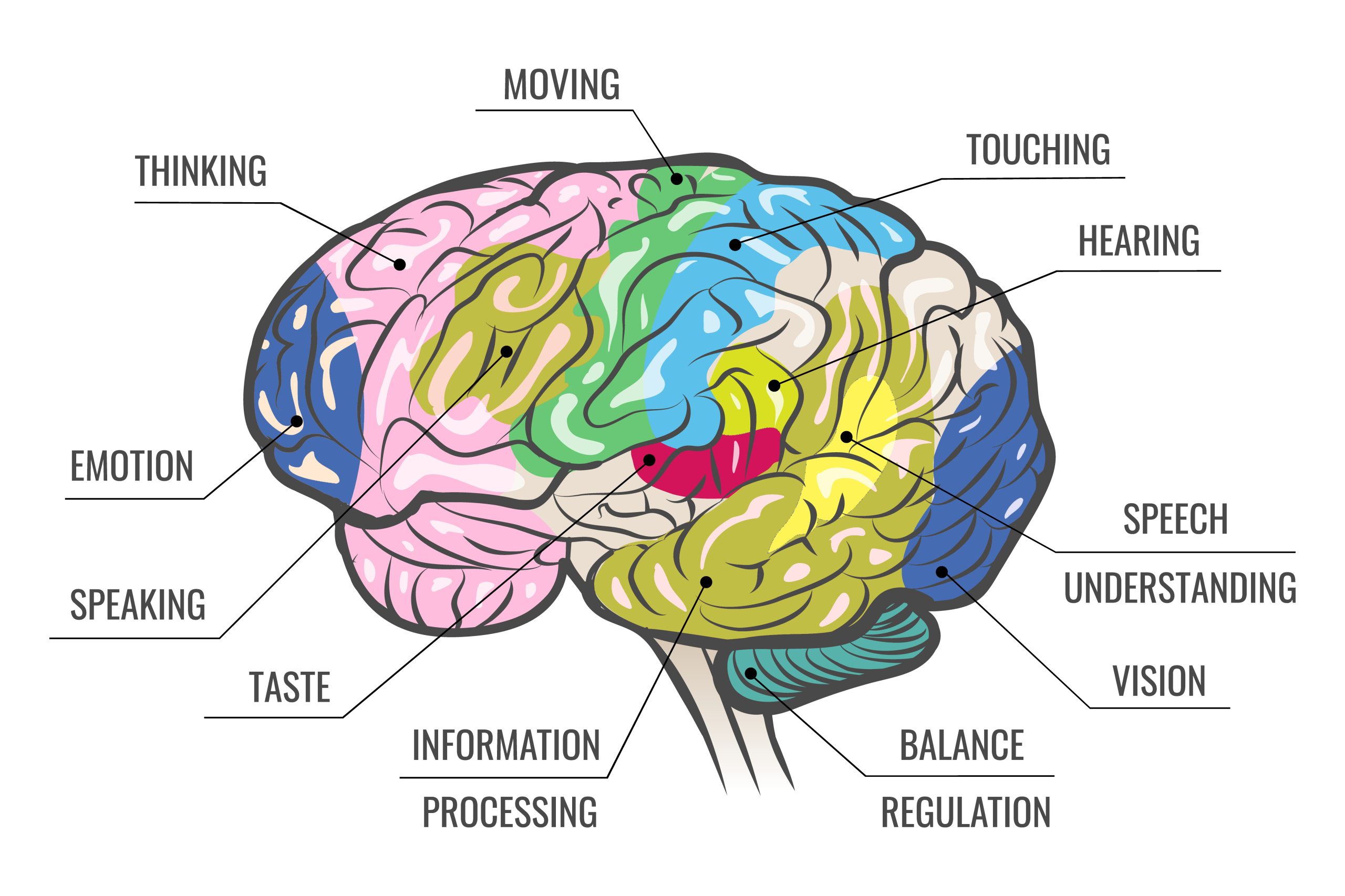
While aging is a major contributing factor to sensory loss, sensory loss can also occur due to a fall, accident, disease, and more.
In the following section, we will explore the five senses and the most common neurological factors contributing to sensory loss.
Sensory Loss in Neurology: Symptoms & Conditions
Vision
The eye, the optic nerve, the optic radiations (or pathways), and especially the occipital lobe primarily govern vision. A decline or loss of vision can be caused by injury, disease, or a neurological event.
Common Symptoms of Vision Loss
Early changes in vision range from blurred vision to complete loss of sight. In many cases, colors may appear washed out or less vibrant. In other cases, individuals may have trouble distinguishing objects in low light.
Patients often report:
- Seeing floaters or small specks drifting across their field of vision.
- Experiencing “tunnel vision” where peripheral vision is lost.
The following are some of the most common causes of neurologic-related visual impairment.
- Stroke
- Alzheimer’s Disease
- Multiple Sclerosis (MS)
- Parkinson’s Disease
- Optic Neuritis
- Brain Tumor
- Leber’s Hereditary Optic Neuropathy (LHON)
- Cortical Blindness
- Neuromyelitis Optica (NMO or Devic’s Disease)
Proactive Measures to limit vision loss symptoms:
- Regular Eye Check-ups: Schedule regular appointments with an ophthalmologist or optometrist to detect potential issues early.
- Protection: Always, and I do mean always, wear sunglasses with UV protection and safety goggles to protect your eyes from harmful rays and potential injuries.
- Limit Screen Time: Prolonged exposure to screens can strain your eyes. Ensure you follow the 20-20-20 rule: every 20 minutes, look at something 20 feet away for at least 20 seconds. Using a blue light filter on your computer screen may be helpful as well.
For more information on vision loss, visit the following Neurology Office article here: Neurological Disorders and Vision Loss
Taste
Primarily controlled by the gustatory cortex, a decline or loss of taste can be caused by injury, disease, or a neurological event.
Common Symptoms of Loss of Taste
Early changes in taste can range from distorted flavors to loss of taste altogether. In many cases, previously enjoyed foods may suddenly become unpalatable. In other cases, the ability to distinguish between sweet, salty, sour, and bitter might be impaired.
Patients often report:
- Experiencing a persistent metallic or bitter taste in the mouth.
- Finding that all foods taste bland or similar, regardless of their actual flavor.
The following are some of the most common causes of neurologic-related taste impairment.
- Stroke
- Multiple Sclerosis (MS)
- Bell’s Palsy
- Parkinson’s Disease
- Dementia
- Illness (including the Coronavirus)
Proactive Measures to Avoid Further Loss of Taste
- Maintain Oral Hygiene: Regularly brush, floss, and get dental check-ups. Poor oral health can directly impact your sense of taste.
- Avoid Smoking: Smoking can dull your sense of taste over time.
- Notify your physician immediately if there is a sudden loss of taste. Consider evaluation with an ENT (Ears, Nose, and Throat doctor.)
Hearing
Primarily controlled by the temporal lobe, a decline or loss of hearing can be caused by injury, disease, or a neurological event.
Common Symptoms of Hearing Loss
Early changes in hearing can range from distorted sounds to complete hearing loss. In many cases, sounds that were once clear may become muffled. In other cases, the ability to discern different tones or pitches may be affected.
Patients often report:
- Experiencing tinnitus, a constant ringing or buzzing in the ears.
- Difficulty understanding speech in noisy environments.
The following are some of the top 5 causes of neurologic-related hearing impairment.
- Auditory Neuropathy Spectrum Disorder (ANSD)
- Acoustic Neuroma
- Multiple Sclerosis
- Stroke
- Ménière’s Disease
- Traumatic Brain Injury (TBI)
- Aging
Proactive Measures to Avoid Loss of Hearing
- Limit Exposure to Loud Noises: Protect your ears from prolonged loud noises. If you are exposed to loud environments regularly, consider using ear protection.
- Regular Hearing Tests: Get your hearing checked regularly to detect early signs of hearing loss.
For more information on hearing loss, visit the following Neurology Office article here: Hearing Loss & Neurology: The Connection
Touch
Primarily controlled by the parietal lobe, a disruption in touch can be caused by injury, disease, or a neurological event.
Common Symptoms of Loss of Touch
Early changes in tactile sensations can range from numbness in certain areas to hypersensitivity. In many cases, a once soft touch may suddenly feel painful. In other cases, patients may not feel anything at all in affected areas.
Patients often report:
- Experiencing a “pins and needles” sensation without apparent cause
- Feeling as though they’re wearing an invisible glove or sock, limiting their sense of touch.
- Numbness, loss of sensitivity, or heightened sensitivity.
- I frequently explain to my patients that I cannot know exactly what they are feeling; the term I like to use is a distortion of sensation.
The following are some of the most common causes of neurologic-related touch impairment.
- Multiple Sclerosis (MS)
- Guillain-Barré Syndrome
- Diabetic Neuropathy
- Carpal Tunnel Syndrome
- Herniated Disk
- Spinal Injury
Proactive Measures to Avoid Loss of Touch
- Engage in exercises that stimulate tactile sensations. Try using textured objects or practicing mindfulness meditation focused on bodily sensations.
- Consult a physician. See a doctor if numbness or hypersensitivity persists, as it may indicate an underlying neurological condition. Checking laboratories, evaluating the nerve function with electrodiagnostic testing, and a thorough neurologic exam can be very helpful in illuminating this process.
Smell
Primarily controlled by the olfactory cortex in the limbic system, a disruption in smell can be caused by injury, disease, or a neurological event.
Common Symptoms of Loss of Smell
Early changes in smell can range from smell distortions to loss of smell altogether. In many cases, a once pleasant scent may suddenly be recognized as unpleasant. In other cases, the ability to identify scent may be diminished or removed.
Patients often report:
- Not being able to distinguish between different types of food based on scent alone.
- Sensing a constant burnt or foul odor even when there is no apparent source for it
The following are some of the most common causes of neurologic-related smell impairment.
- TBI (Traumatic Brain Injury)
- Brain Hemorrhage or Tissue Damage
- Parkinson’s Disease
- Alzheimer’s Disease
- Huntington’s Disease
- Epilepsy
- Multiple Sclerosis (MS)
- Illness (Coronavirus)
Proactive Measures to Avoid Loss of Smell
- Avoid Smoking: Smoking can impair your sense of smell.
- Safety First: Use protective gear when working with chemicals or in environments where there might be irritants in the air.
Sensory Loss Diagnosis & Management
For any changes in sensory ability, it is recommended to see your primary care physician (PCP) right away. Several reasons for sensory changes might be physiological or temporary, stemming from minor ailments such as infections, colds, or even some medications. Your PCP can help rule out these more common causes.
For further evaluation, a neurologist can perform diagnostic testing ranging from MRI to scans to EMG to help identify the origin of symptoms. Neurologists specialize in diagnosing and treating disorders of the nervous system, which includes the brain, spinal cord, and peripheral nerves. From there, a tailored treatment plan can be established.
For more information on diagnosis and testing, visit the following Neurology Office article below: Neurology and Medical Imaging: What You Need to Know
A Message From Dr. Kandel
“A distortion of sensation is a warning sign from the nervous system that something is not right. Like with any other medical problem, evaluating this and addressing this as quickly as possible is the correct approach to treating these processes. Delaying diagnosis and treatment may lead to more serious problems and even a more permanent process. Don’t take your symptoms for granted. Listen to your body… it is telling you something!”
Feel free to share this with the people in your life who may benefit from this information! For more insights on neurology, check out our weekly tips on our Neurology Office Facebook page.
“To Cure Sometimes, To Heal Often, To Comfort Always”
Neurology Office, Joseph Kandel M.D. and Associates
“Concierge medicine without the concierge price”













